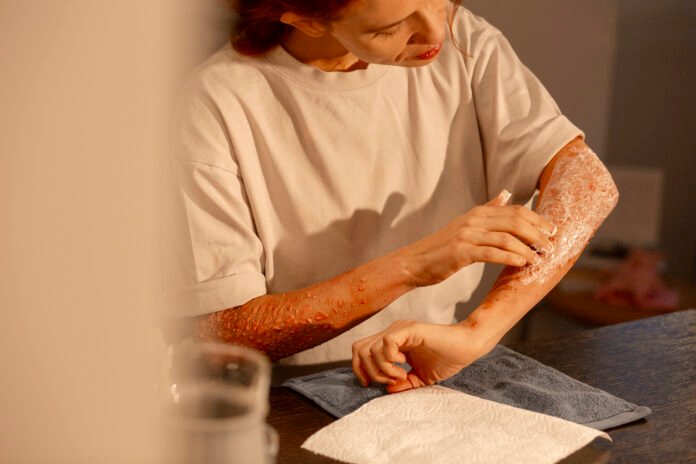
Have you ever met a type 2 diabetic person? You may notice that people with type 2 diabetes often experience skin health problems. Type 2 diabetes and skin health are closely related. Diabetes affects your skin in many ways. Therefore, people with type 2 diabetes have to pay more and more attention to their skin health and deal with all the skin related issues with great care. Poor wound healing, skin ulcers and cracked skin are the early signs of type 2 diabetes that are shown by your skin.
Yes, skin health issues are the first symptoms and visible signs of type 2 diabetes. Even if you already have skin problems, type 2 diabetes can make them worse. In addition, new skin health problems also occur.
Overview
Studies show that type 2 diabetes actually has a great impact on your body’s functions especially it changes the ways through which your body uses glucose and sugar. A naturally occurring hormone, insulin, in your body helps regulate the amount of sugar in your blood. But sometimes, the insulin production gets disturbed due to several factors and lower production of insulin causes higher levels of blood sugar that results in type 2 diabetes. It also happens when your body can’t respond to insulin effectively. The persistently high glucose level is known as hyperglycemia. When glucose levels remain high in your blood over time, it starts damaging your body’s structure and functions. The condition makes you more prone to infections, especially skin infections, slows down wound healing and causes damage to your blood vessels.
These factors are not the end of the story but they open a door that leads you to a range of skin problems caused by type 2 diabetes. Let’s have a deep look!
Causes of Diabetes-Related Skin Diseases
Some factors contribute a lot in making you more prone to the skin problems especially if you’re a diabetic person:
- Inactive White Blood Cells: Type 2 diabetes makes your white blood cells less active or inactive. Therefore, they cannot defend against infections.
- Damaged Blood Vessels and Nerves: Type 2 diabetes causes damage to your blood vessels and nerves that leads to disturbance in blood flow and blood circulation throughout your body especially towards your skin. Poor blood circulation causes an abrupt change in collagen that often affects the appearance, texture and healing ability of your skin.
- Damaged Nerves: Type 2 diabetes often causes damage to your nerves which is also known a diabetic neuropathy. The condition makes you unable to notice injury and wounds on skin. The uninjured injuries turn into severe complications, when not treated well.
- Damaged Skin Cells: Type 2 diabetes causes damage to your skin cells that create problems in your sweating ability. This factor increases the sensitivity to pressure and temperature in your skin.
What are the Symptoms to Watch for?
According to research, a large number of diabetic people experience diabetes-related skin diseases. Therefore, it is necessary for you to watch for such skin conditions and other symptoms, if you’re diabetic.
Common symptoms of diabetes-related skin conditions include:
- Wounds or injuries that heal slowly and become an entryway to other infections due to slow healing.
- Injuries or cuts that become infected.
- Changes in texture and color of skin.
- Irritating injuries or swellings around the insulin injection sites.
Studies also show that diabetes contributes a lot in making your immune system less active when there’s a need for a stronger immune system at infection fighting sites.
In addition, due to weak immunity, fungi, bacteria and other pathogens invade your body easily and can be removed with great difficulty.
Types of Bacterial and Fungal Infections Affecting Your Skin
Sometimes, certain fungi and bacteria also cause a few skin conditions especially if you have type 2 diabetes.
Common examples are:
Bacterial Infections
Many skin diseases are caused by bacteria. Most common types of bacteria that cause the skin conditions are Staph or Staphylococcus.
They cause some bacteria skin infections, such as:
- Infections around your nails.
- Boils.
- Deep skin infections that reach inside tissues.
- Swelling in the eyelids known as styles.
- Hair follicle infection known as folliculitis.
- You can trace the following in infected region:
- Swelling.
- Pain.
- Darker skin or redness.
- Warmth.
Persistent high levels of blood sugar is the leading cause of severity of these symptoms. Broken skin allows bacteria to enter the body that makes infections worse and symptoms severe.
Fungal Infections
When yeast or fungus grow and spread in the specific area of the body, fungal infection occurs. Like bacteria, fungi also can infect anyone. But if you’re diabetic, you’re more susceptible to fungal infections. People who are living with type 2 diabetes and also unable to manage their blood sugar level are more likely to get infected by fungal skin infections.
The most common cause of fungal infractions is a yeast-like fungus named Candida albicans. This fungus causes infections having the following symptoms:
- Dry scales with blistering.
- Release of cottage cheese like white discharge from blisters.
- Itchy, swollen and red or discolored skin.
The following areas are more prone to get infected with the yeast-like fungus:
- Corners of mouth.
- Warm folds of the skin.
- Underneath the skin of the penis.
- Under the breasts.
- Inside the armpits.
- Inside the groin.
Some other skin infections like ringworm, athlete’s foot and jock itch are also fungal infections. They cause itching and spread the symptom. They can be treated with prescription medications.
Studies show that type 2 diabetes causes changes in your small blood vessels which are supplying nutrients to your skin resulting in skin irritations in specific areas.
Types of Diabetes-Related Skin Conditions
Here are some types of type 2 diabetes-related skin conditions that affect your skin health.
Diabetic Dermopathy
The skin condition gets noticed when brown, scaly patches appear on the skin especially on shins. These are the hallmark of diabetic dermopathy and also known as “shin spots”. They are in circular or oval shape.
According to studies, more than 50% of diabetic people experience diabetic dermopathy. When type 2 diabetes causes damage to small blood vessels that transport nutrition to your skin cells. Although the condition is not life-threatening it becomes worse when left untreated and leads to severe complications. People having neuropathy, kidney disease or retinopathy are more likely to develop this condition. So, when you notice these changes in your skin, consult your doctor as soon as possible to get an effective treatment pl;an.
Necrobiosis Lipoidica Diabeticorum (NLD)
The appearance of light brown, circular or oval patches on the skin is categorized as NLD. However, its patches are larger and deeper than diabetic dermopathy. No doubt, it is a rare condition that doesn’t occur commonly and often affects the people with type 1 diabetes.
- Its patches:
- Are itchy.
- Often looks like a shiny scar.
- Appear as firm, reddish-brown papules.
- First appear on the lower leg but sometimes on the face, arms and scalp.
- Affect both sides of the body.
- Also cause ulcers.
- Develop thinner, weaker and waxy skin in the center.
Doctors still are trying to find out what is the real cause of NLD, but all in vain. However, some studies suggest that it occurs due to breakage in collagen tubes. There’s no specific treatment for the condition but compression therapy helps manage symptoms.
Digital Sclerosis
Potentially stiff, tight, thick and waxy skin on your fingers and is the first sign of digital sclerosis. It also affects the joints and makes them harder to move. Every one person out of three in type 1 diabetic oriole experience these symptoms.
In addition, the risk of the condition increases when your blood sugar levels remain high persistently.
Applying lotions and moisturizers on affected areas can help manage the symptoms. You also have to manage our blood sugar level to fight against the condition.
Disseminated Granuloma Annular
The appearance of ringed shapes, rashes or raised bumps in the skin is called disseminated granuloma annular. The ski time of rashes are usually red-brown, light or red. But sometimes, the area may be the same color as your skin. The common targets of this condition are hands and feet. The condition is not harmful and easy treatment options are available.
Acanthosis Nigricans (AN)
The condition occurs when the pigmented substances accumulate in your skin-folds. Its patches are:
- Velvety in nature.
- With ill-defined borders.
- Thicker and darker than surrounding skin.
The most affected areas include:
- Knees.
- Groin.
- Elbows.
- Neck.
- Armpits.
Insulin resistance is the leading cause of AN. This is also known as an early sign of type 2 diabetes. obese and overweight people are commonly affected with the condition. Losing weight can help treat the skin condition.
Diabetic Blisters
Type 2 diabetes often causes blisters on skin that usually look like burns. The condition is common in people who have diabetic neuropathy. The rashes appear on:
- Legs and firearms.
- Back of fingers and toes.
- Hands and feet.
Rashes are not ever-secret and often tend to heal on their own. You can reduce the risk of the condition by managing your blood sugar levels.
Best Treatment Options for Diabetic Skin Conditions
The first thing you can do to treat your diabetic skin condition is to manage your blood glucose level.
Other important treatment options include:
- Over-the-counter (OTC) treatments.
- Prescription treatments.
- Alternative remedies.
- Lifestyle changes.
- Over-the-Counter Remedies
- Certain diabetes skin conditions can be treated with OTC remedies, such as:
- Moisturizers and lotions are used to remove skin dryness.
- Nonprescription anti-fungal are used to disinfect the skin.
- Topical steroid medications are used to treat rashes and blisters.
Prescription Medications
When the condition doesn’t get better OTC medications, your doctor may prescribe the following:
- Stronger anti-fungal medications to disinfect the skin.
- Insulin therapy and other drugs to manage blood glucose levels.
- oral or topical antibiotics to heal the wounds and rashes.
Some specific treatments are used to treat specific conditions. For example:
- Doctors usually pierce and drain the blisters for treating caruncles, a bacterial infection. Sometimes, they prescribe antibiotics.
- Similarly, for NLD, doctors sometimes describe corticosteroids, light therapy or other uncommon drugs. For treating granuloma annular, they recommend photo-therapy and steroids.
Alternative Remedies
Some diabetes-related skin conditions are treated with non-drug remedies, like:
- Aloe vera is applied topically on rash and blisters.
- Talcum powder is considered effective for preventing itching and friction in skin folds.
- Skin specialized lotions are used for reducing dryness and itching.
However, avoid using any new remedy for skin condition without your doctor’s consultation. Because all drugs and even natural herbal supplements or ointments can interfere with the medications you’re taking for relieving the symptoms.
Lifestyle Changes
Some lifestyle changes can impact and help you manage skin conditions caused by diabetes.
- Take measures to manage your blood sugar levels.
- Monitor your blood sugar regularly.
- Take a diabetes-friendly diet.
- Follow a regular exercise routine.
Type 2 diabetes related skin conditions can be managed by:
- Treating wounds and ashes immediately.
- Avoid hot baths as they can dry out your skin.
- Taking prescribed medications to prevent dryness.
- Keeping your home humid during dry months.
- Inspecting your skin-folds and feet regularly especially if you’re experiencing symptoms of neuropathy.
- Avoiding scratching skin as it causes breaking the skin that makes you prone to infections.
However, talk to your doctor before making any change in your diet or exercise routine.
Conclusion
Type 2 diabetes is the leading cause of many skin conditions. This means type 2 diabetes and your skin health are interlinked. If you want to avoid any skin condition while having type 2 diabetes, you need to manage your blood sugar levels. This can help you prevent skin problems that arise with diabetes.
In addition, several skin conditions predict that you’re near to having diabetes. So keep an eye on your ski health. This will make you informed about any changes in your skin.
Various treatment options are used to treat skin conditions caused by diabetes. But the best one is recommended by your doctor. Whenever you notice any new or worsening symptoms, contact your doctor immediately and try to review your diabetes treatment plan along with tracking your blood sugar levels. Seeking immediate medical advice can help treat skin ulcers and cancer.